Trauma rarely stays where the mind expects it. Long after a difficult event has passed, sensations may linger in the shoulders, the gut, the hips, or the chest. This is not imagination. The body can continue responding to past experiences through the nervous system, and the way trauma is experienced in the body often shows up in posture, breathing, and patterns of physical tension that can feel impossible to shake.
For women looking for compassionate, holistic residential trauma recovery support, understanding the somatic map is often the first meaningful step toward deeper healing. This guide walks through where trauma is stored in the body, the science behind those patterns, and the therapeutic approaches that help release stored trauma in lasting ways. The goal is not to diagnose pain but to make sense of it, so the road ahead feels less mysterious and more navigable.
Why the Body Remembers What the Mind Tries to Forget

When someone goes through traumatic events, the brain’s usual memory-processing systems can become overwhelmed. Instead of filing experiences neatly into the past, the brain may store fragments, sensory snapshots, and reactive patterns that can trigger intense physical reactions later. The mind may move on, yet the body can continue reacting.
Researchers have found that trauma can create lasting changes in nervous system functioning by altering neural pathways and stress response patterns. These changes can persist for years, shaping how someone perceives daily situations and reacts to perceived threats. The phrase “the body keeps the score” is often used to describe this process, meaning the nervous system continues to respond even when conscious memory has faded.
Safe, Supportive Trauma Treatment for Women
Heal from trauma in a compassionate, women-centered environment with evidence-based therapies designed to help you feel safe, regain control, and move forward with confidence.
How Trauma Becomes Reflected in the Body
Research shows that trauma affects the brain and nervous system, which in turn can influence muscle tension, breathing patterns, pain sensitivity, and physical symptoms over time. Some therapeutic frameworks describe this as the body “holding” trauma, but this reflects changes in stress response rather than literal storage of memory in tissues.
Trauma-related stress can lead to chronic physical symptoms such as muscle tension, fatigue, and digestive issues. When stress responses persist, they influence how a person breathes, moves, and rests. Many trauma survivors describe a sense that their bodies are reacting in ways their conscious mind has not yet learned to read.
Where Trauma Is Stored in the Body: A Full Somatic Map
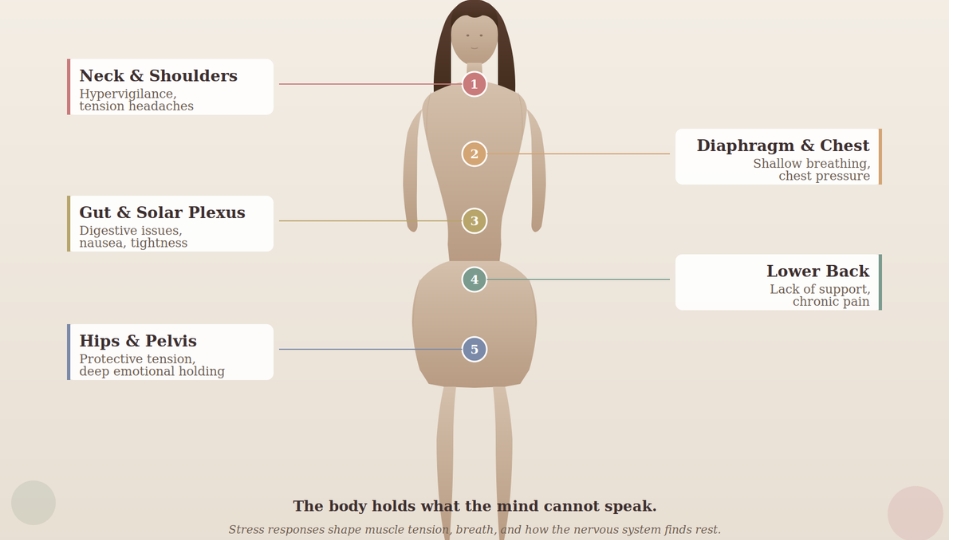
Different stress responses tend to show up in different areas, creating patterns of physical pain and tension. While each person’s somatic landscape is unique, common holding patterns can emerge. The associations below are descriptive and not diagnostic.
The Neck and Shoulders
The neck and shoulders frequently carry the weight of hypervigilance. People who have experienced trauma often describe a sense of always being braced for something. Chronic muscle tension in the trapezius, jaw, and upper back is common, and it can lead to tension headaches that persist despite rest.
This area also reflects patterns of physical bracing. When responsibility, fear, or vigilance becomes habitual, the shoulders rise and stay raised.
The Diaphragm and Chest
The diaphragm sits at the crossroads of breath and emotion. When someone is under emotional distress, breathing becomes shallow, and the diaphragm tightens. Over time, this restricted breathing pattern can feel normal, even though it limits the body’s natural calming response.
Trauma-related stress can contribute to tension in the diaphragm, hips, and lower back. A constricted diaphragm may show up as pressure in the chest, frequent sighing, or difficulty taking a full breath.
The Hips and Pelvis
The hips are often associated with long-term protective tension. Some trauma survivors, including those with chronic stress or sexual trauma histories, may experience tightness in the hip flexors, lower back, or pelvic floor.
For many trauma survivors, releasing tension in the hips through somatic therapy or trauma-informed bodywork may bring emotional waves. This can reflect the connection between physical tension and emotional processing, though it is not a precise map of specific experiences.
The Lower Back
Lower back tension can be tied to themes of support and safety. When someone has lived without reliable emotional or financial support, the lower back often compensates. Chronic pain in this area is among the most reported somatic symptoms in adults with histories of complex trauma and CPTSD.
The Gut and Solar Plexus
The gut is sometimes called the second brain for good reason. Many people who have experienced trauma struggle with digestive issues, including irritable bowel syndrome, nausea, and food sensitivities. The gut-brain connection means emotional stress can directly affect digestion.
The solar plexus area may hold sensations of tightness or discomfort during stress or anxiety, reflecting nervous system activation rather than a fixed emotional meaning.
The Throat and Jaw
The throat is where silenced truths tend to settle. Tightness, difficulty swallowing, and jaw clenching can reflect years of unspoken words. This holding pattern is common among people whose voices were dismissed, controlled, or punished, including survivors of coercive and emotionally abusive relationships.
Holding Patterns at a Glance
The table below summarizes common stress-related patterns. It is meant as a starting place rather than a fixed diagnosis.
| Body Region | Common Holding Patterns | Possible Emotional Themes |
|---|---|---|
| Neck and shoulders | Chronic muscle tension, tension headaches, jaw clenching | Hypervigilance, stress |
| Chest and diaphragm | Shallow breathing, chest pressure, sighing | Emotional distress |
| Hips and pelvis | Tightness, pelvic floor tension | Protective tension patterns |
| Lower back | Chronic pain, stiffness | Stress, muscle guarding |
| Gut and solar plexus | Digestive issues, nausea, irritable bowel syndrome | Anxiety, gut-brain interaction |
| Throat and jaw | Tightness, difficulty swallowing | Stress, tension |
How Trauma Rewires the Nervous System
Trauma does not only affect feelings. It reshapes the functioning of the nervous system, which is why somatic symptoms can feel so persistent.
The Three-Branch Stress Response
After trauma, these systems can become dysregulated. The body may swing between hyperarousal and shutdown, sometimes within the same day. This dysregulation sits at the heart of many post-traumatic stress disorder symptoms in women, and it explains why trauma symptoms can feel both relentless and unpredictable.
The Amygdala and Hyperactivity Loop
Heightened threat detection and reduced regulation can keep the body in constant alert. This shows up as increased heart rate, elevated blood pressure, and reduced heart rate variability.
How Stored Trauma Affects Physical Health
The connection between trauma and physical health is well-documented. Individuals with trauma histories often experience higher rates of physical health problems compared to those without such experiences.
The Adverse Childhood Experiences (ACEs) study found a strong relationship between childhood trauma and adult health outcomes, including increased risk of cardiovascular disease, chronic illness, and mental health conditions.
When emotional stress goes unaddressed, the body finds other ways to communicate distress. Various physical symptoms, from chronic fatigue to tension headaches, can be signs that unresolved trauma is asking for attention. Recognizing these patterns is part of knowing when trauma therapy may be needed.
Childhood Trauma and Adult Holding Patterns
Childhood is a particularly vulnerable window for stress. A young nervous system adapts to overwhelming experiences, and those adaptations can persist into adulthood.
Adults shaped by childhood trauma often describe a sense of always being on edge or shut down. The patterns set in early life can become the body’s default settings, even after circumstances change. This is one reason why understanding how trauma affects women differently is essential for tailoring care.
Emotional Distress and the Body’s Reaction
The mind and body are deeply interconnected. Emotional pain often translates into physical discomfort. Stress can lead to muscle tension, increased heart rate, and shallow breathing.
Research shows that unresolved emotions can trigger physiological responses that affect different parts of the body. If these stress responses become habitual, they can contribute to long-term health issues. Recognizing this loop is essential for healing trauma at the root rather than only managing surface-level trauma symptoms.
Chronic Stress and Cardiovascular Strain
Prolonged stress floods the system with cortisol and adrenaline. This sustained chemical bath can damage heart tissue and lead to chronic inflammation. People living with traumatic stress often show patterns of cardiovascular strain that mirror their internal experience.
Blood Pressure and Heart Rate Variability
Sustained stress activation can lead to elevated blood pressure and reduced heart rate variability, reflecting long-term nervous system strain.
The Gut Brain Connection
The gut-brain connection explains why digestive issues are common among trauma survivors. The vagus nerve carries signals between the gut and brain, allowing emotional stress to influence digestion.
The insular cortex plays a role in processing bodily sensations, which may contribute to heightened awareness of physical symptoms.
Mental Health Symptoms Linked to Stored Trauma
Trauma affects both physical and mental health. Common patterns include anxiety, depression, intrusive memories, and difficulty trusting one’s perceptions.
For women living with overlapping anxiety, depression, and PTSD, the connection between psychological and physical symptoms can feel especially heavy. Addressing one without the other often leaves recovery incomplete, which is why integrated care matters so much.
When stored trauma surfaces as chronic anxiety that interferes with work, our overview of whether anxiety qualifies as a disability under the ADA explains the workplace protections that may apply
Approaches to Healing Trauma Through the Body
Healing trauma often requires helping the body experience safety and regulation.
EMDR Therapy and Bilateral Stimulation
EMDR therapy is an evidence-based treatment for trauma and PTSD. It uses bilateral stimulation to help process traumatic memories so they become less distressing.
For people who want a fuller picture of structured cognitive approaches alongside EMDR therapy, comparing it with CBT for PTSD can help clarify which methods feel like the right fit.
Somatic Experiencing
Somatic experiencing focuses on the body’s response to threat and helps complete the stress cycles that became frozen during traumatic experiences. Through gentle attention to physical sensations, it allows the nervous system to discharge stored stress safely. This approach is particularly useful when talk therapy alone has not produced lasting change.
Yoga and Movement-Based Practices
Movement-based therapies such as yoga and somatic exercises, along with mindfulness practices like meditation, may support nervous system regulation.
A consistent movement practice can support trauma recovery by:
- Lowering baseline arousal
- Improving interoception
- Releasing tension
- Building tolerance for sensation
- Strengthening body awareness
Trauma-Informed Bodywork
Therapies like somatic experiencing and trauma-informed bodywork provide targeted approaches for addressing unresolved emotional pain. They help individuals explore the underlying causes of physical discomfort, which can be a critical step in releasing trauma that has settled into tissue. When delivered as part of trauma-informed care, this work supports deeper healing without retraumatizing the client.
For people whose stored trauma traces back to early attachment wounds, our guide on how therapy for abandonment trauma works explains how somatic and relational approaches fit together in a treatment plan.
How the Body’s Response Begins to Soften
As the nervous system learns new patterns, the body’s response to stress may shift. Common changes include:
- Greater capacity to feel emotions without becoming overwhelmed
- More restful sleep and steadier energy
- Easier breathing and a softer diaphragm
- Reduction in chronic pain and digestive issues
- Increased curiosity about the body rather than fear of it
Many people notice these changes during and after structured care. A look at what happens after trauma treatment can offer a more complete view of how recovery unfolds over time.
Building a Personalized Recovery Path
No two people store trauma in the same way, which is why one-size-fits-all programs often fall short. A thoughtful recovery path blends several modalities, honors the body’s pacing, and addresses both emotional wounds and physical symptoms. For many women, residential or outpatient trauma-focused care for women offers the structure and community that home life cannot easily provide.
Programs that integrate EMDR therapy, somatic therapy, movement, and skilled clinical support tend to offer the most durable results. Working with clinicians experienced in trauma symptoms helps ensure that the pace of healing matches the body’s readiness, rather than rushing through layers of stored experience. For survivors of relational harm, exploring the long-term effects of narcissistic abuse and the link between trauma and eating disorders in women can also illuminate why a layered approach matters.
Body-based work pairs well with cognitive approaches like cognitive behavioral therapy for abandonment issues, which targets the thought patterns that keep the nervous system on alert.”
Where Trauma is Stored in the Body: Frequently Asked Questions
How long does it take to release stored trauma?
There is no fixed timeline. Some people notice meaningful shifts within weeks of beginning targeted work, while others, especially those with complex or layered histories, find that recovery unfolds over months or longer. What matters more than speed is consistency, safety, and a treatment plan that respects the body’s pacing. Trauma recovery tends to move in waves rather than a straight line.
Can trauma really cause physical pain even years later?
Yes. Trauma and chronic stress can contribute to ongoing pain, tension headaches, digestive issues, and other physical symptoms long after the original events. The nervous system can remain in a heightened state of stress, which often manifests physically. Addressing the underlying stress patterns frequently helps ease symptoms that have not responded to medical treatment alone.
Is EMDR therapy better than talk therapy for trauma?
Both approaches have value, and many people benefit from a combination. EMDR therapy is an evidence-based option for processing traumatic memories, while talk therapy can build insight, coping strategies, and a strong therapeutic relationship. The right approach depends on the individual, the type of trauma, and the goals of care.
