Do I need trauma therapy? It is a common internal monologue:“I wasn’t in a war. I didn’t survive a plane crash. I had a roof over my head growing up. So why do I feel like this?”
When we think of trauma, our minds often jump immediately to Post-Traumatic Stress Disorder (PTSD) caused by life-threatening catastrophes. Because of this limited definition, countless people spend years struggling with anxiety, depression, and self-doubt, telling themselves that their experiences “weren’t bad enough” to warrant help. They believe they should be able to handle it on their own.
But pain is not a competition, and you do not need a specific diagnosis to deserve support.
The reality is that trauma is not always loud. It can be quiet, cumulative, and deeply ingrained in how you navigate the world. Many people living with unresolved trauma function at a high level, using exhaustion as a coping mechanism while their mental health quietly deteriorates behind the scenes.
If you feel stuck in patterns you can’t break, it may be time to look for the signs you need trauma therapy (beyond PTSD). You aren’t“broken”, you might just be carrying a burden you were never meant to hold alone.
Safe, Supportive Trauma Treatment for Women
Heal from trauma in a compassionate, women-centered environment with evidence-based therapies designed to help you feel safe, regain control, and move forward with confidence.
Defining Trauma: It’s Not Just the Event

To understand if you need help, we first have to redefine what trauma actually is. We often confuse trauma with the traumatic event itself, the accident, the assault, or the disaster.
However, trauma experts define it differently: Trauma is not what happens to you; it is what happens inside of you as a result of what happened.
Trauma occurs when an experience overwhelms your internal resources and your ability to cope. If you did not have the support, safety, or tools to process an event when it happened, that energy gets locked in your nervous system.
While “Big T” trauma (acute, life-threatening events) is widely recognized, “Little T” trauma (cumulative, relational, or developmental stressors) can be just as damaging over time. These experiences often fly under the radar because they are normalized by society or families.
You may benefit from trauma therapy if you have experienced:
- Childhood Emotional Neglect: Growing up with parents who were physically present but emotionally unavailable or critical.
- Sudden or Complicated Grief: Losing a loved one, a job, or a sense of identity abruptly.
- Medical Trauma: Experiences with chronic illness, invasive surgeries, or dismissive healthcare providers.
- Toxic Relationships: Long-term exposure to narcissistic abuse, gaslighting, or emotional manipulation.
- Systemic Stress: Living with the daily, grinding stress of discrimination, poverty, or a hostile work environment.
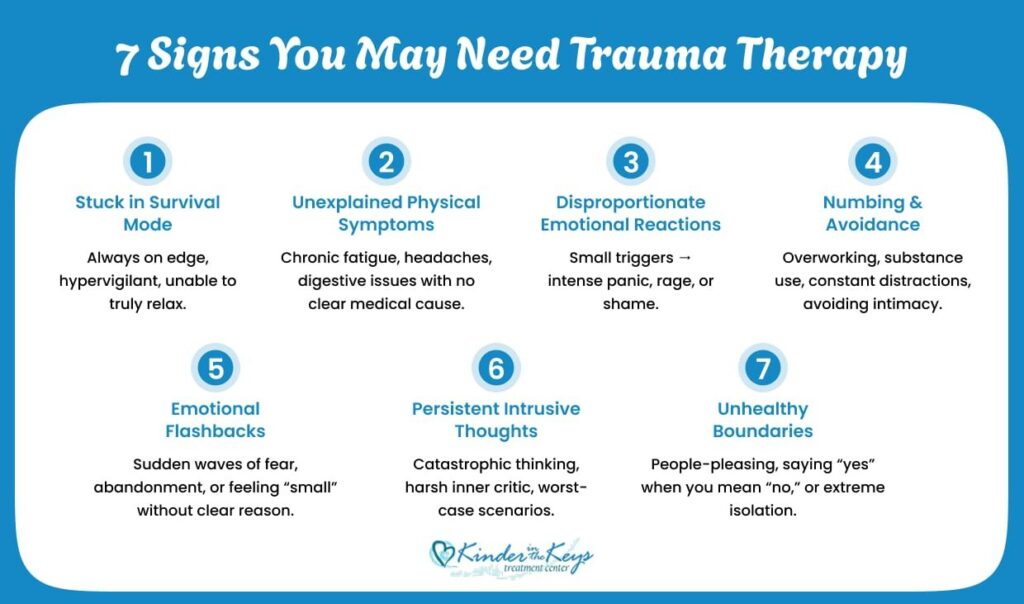
7 Signs You Need Trauma Therapy (Beyond PTSD)
Trauma is often described as a “silent epidemic” because so many of its symptoms mimic personality traits or other conditions. You might label yourself as a “control freak,” a “worrier,” or simply “oversensitive,” when in reality, you are dealing with a biological response to past pain.
Here are seven key indicators that your mind and body are trying to process unresolved trauma.
You Are Stuck in “Survival Mode” (Hypervigilance)
If you feel like you can never truly relax, even when you are sitting on your couch in a safe home, you may be stuck in a state of hypervigilance. You might find yourself constantly scanning the room for danger, flinching at loud noises, or feeling an intense need to monitor the moods of everyone around you. This is your nervous system stuck in the “On” position. Because it was once dangerous for you to let your guard down, your body has not yet received the message that the threat is gone.
You Experience Unexplained Physical Symptoms
We often think of trauma as a purely mental struggle, but trauma is physiologically stored in the body. When emotional distress is not processed, it converts into physical pain.
You might struggle with chronic fatigue, digestive issues like IBS, or persistent tension headaches that medical doctors cannot seem to explain or cure. If you have treated the physical symptoms for years with no relief, it is often a sign that the root cause is emotional.
Your Emotional Reactions Feel Disproportionate
Do you find yourself going from zero to one hundred in a matter of seconds? Perhaps a minor disagreement with a partner sends you into a spiral of panic, or a small mistake at work triggers intense shame or rage.
When your emotional reaction does not match the severity of the current situation, it usually means the present moment has triggered an old wound. You aren’t just reacting to the spilled coffee; you are reacting to a lifetime of feeling unsafe or criticized.
You Rely Heavily on Numbing and Avoidance
It is natural to want to move away from pain, but when avoidance becomes your primary lifestyle, it limits your life. This doesn’t just mean avoiding the scene of an accident. It manifests as avoiding intimacy because it feels dangerous, avoiding silence by constantly consuming media, or avoiding emotions through substance use, overeating, or workaholism. If you cannot sit alone with your thoughts without feeling the need to numb out, you are likely running from unprocessed trauma.
You Suffer from “Emotional” Flashbacks
When we hear the word flashbacks, we typically imagine a cinematic scene where a person hallucinates that they are back in a war zone. However, complex trauma often manifests as emotional flashbacks. You may not hallucinate a visual memory, but you will suddenly be hijacked by intense feelings of fear, abandonment, or “smallness” that belong to the past. You might feel like a helpless child in a grown adult’s body, unable to explain why you suddenly feel unsafe.
You Have Persistent Intrusive Thoughts
Trauma changes the way your brain predicts the future. If you have been hurt before, your brain tries to protect you by imagining every possible worst-case scenario. This leads to intrusive thoughts that are repetitive, disturbing, and difficult to control. You might be plagued by a harsh inner critic that attacks your self-worth or catastrophic thinking that convinces you disaster is always right around the corner.
You Struggle to Maintain Healthy Boundaries
Trauma impacts your ability to trust yourself and others. This often swings to one of two extremes. You might have rigid, porous walls where you isolate yourself and refuse help (the “flight” response).
Conversely, you might have non-existent boundaries, where you constantly people-please, say “yes” when you want to say “no,” and stay in toxic relationships (the “fawn” response). Inability to protect your own energy is a hallmark sign that you need support in rebuilding your sense of self.
Why “Talking It Out” Isn’t Always Enough
If you have tried traditional talk therapy but still feel stuck, you are not failing. Standard therapy engages the logical brain, but trauma lives in the body. You cannot simply “think” your way out of a nervous system response.
While logic helps you understand your history, it often fails to stop the physical symptoms of anxiety. True healing requires a “bottom-up” approach, calming the body first so the mind can follow. This is why specialized trauma therapy is essential; it addresses the physiological roots of your pain, not just the story behind it.

How to Know If You Need Trauma Therapy
Deciding whether you need trauma therapy isn’t always obvious, especially when you’ve spent years learning to push through. But the question isn’t only “do I have symptoms?” It’s whether those symptoms are quietly running your life.
Ask yourself honestly: Are you avoiding people, places, or situations because they don’t feel safe, even when logically you know they are? Is sleep something you dread or can’t sustain? Do you find yourself disconnecting mid-conversation, losing track of the present, or feeling emotionally numb around people you love?
Trauma doesn’t always look like a crisis. Sometimes it looks like snapping at your partner for no clear reason, struggling to concentrate at work, or feeling a persistent low-grade dread you can’t explain. If your past is quietly shaping how you function today (in your relationships, your productivity, your body, your sense of safety) that’s worth paying attention to.
You don’t need to have experienced something “bad enough” to deserve support. If it affected you, it matters.
When to Seek Help for Trauma
There’s a common hope that time will do the work, that if you just give it long enough, things will settle. Sometimes they do. But there are specific signs that waiting is no longer serving you.
- Symptoms aren’t improving on their own. If months have passed and you’re still experiencing flashbacks, hypervigilance, emotional numbness, or intrusive thoughts, your nervous system is stuck in a pattern it can’t resolve without support.
- You’re using substances to cope. Alcohol, cannabis, or other substances can temporarily quiet trauma responses, but they prevent the nervous system from actually processing what happened. If you’re relying on something external to feel okay, that’s a significant signal.
- Your relationships keep breaking down. Trauma often lives in connection. It can make intimacy feel threatening, trust feel impossible, and conflict feel catastrophic. If patterns keep repeating across relationships, trauma may be driving them.
- The past keeps intruding on the present. When a smell, a tone of voice, or an ordinary moment pulls you back into something that happened years ago, and your body responds as if it’s happening now, that’s not a memory problem. That’s a trauma response that needs professional attention.
Signs You Need Trauma Counseling (Not Just Self-Help)
Self-care matters. Journaling, movement, breathwork, community, rest: these things are genuinely helpful, and they’re nothing. But there’s a real difference between what self-care can support and what it cannot treat.
Self-care can help you manage day-to-day stress, build resilience, and maintain well-being when your nervous system is basically regulated. It struggles and often fails when trauma is the underlying issue.
Here are the signs that you’ve moved beyond what self-help can reach:
- You’ve tried and the symptoms keep returning. You’ve done the journaling, the meditation, the podcasts. You feel better briefly, then something triggers you and you’re back at the start. This cycle isn’t a willpower problem. It’s an indicator that the trauma hasn’t been processed, only managed.
- Your window of tolerance is narrow. You’re either emotionally flooded (overwhelmed, reactive, unable to think clearly) or completely shut down and disconnected. Swinging between these states is a sign your nervous system needs more than lifestyle support.
- You dissociate regularly. Zoning out, feeling unreal, losing time, or watching yourself from outside your body are dissociative symptoms that self-help cannot safely address.
- Physical symptoms have no medical cause. Chronic pain, digestive issues, fatigue, or tension that your doctor can’t explain may be trauma stored in the body, something talk-based self-help rarely reaches.
- You’re avoiding life to stay functional. If your coping strategy is making your world smaller (fewer relationships, fewer risks, fewer situations that might activate you) that’s not management. That’s contraction. Professional trauma counseling can help you expand again, safely.
What Happens When You Start Trauma Therapy?
One of the biggest barriers to starting isn’t doubting that therapy works. It’s not knowing what it will actually feel like to walk into it. Uncertainty about the process keeps a lot of people on the fence far longer than they need to be.
Here’s what you can generally expect:
Your first sessions won’t involve being asked to relive everything. A skilled trauma therapist will spend time building safety and understanding your history before any deeper processing begins. You won’t be pushed faster than your nervous system can tolerate, because that’s not how effective trauma therapy works.
Over time, depending on the approach, you’ll begin to work with how trauma lives in your thoughts, your body, and your patterns of relating. For some people, this looks like structured cognitive work, examining the beliefs trauma created and building more accurate, compassionate ones. You can read more about what that looks like in CBT for trauma. For others, it’s more somatic, relational, or narrative-based.
Therapy often feels uncomfortable before it feels relieving. That’s not a sign that something is wrong. It’s a sign that things that were buried are finally being met. Most people begin to notice meaningful shifts within weeks to months, not years.
If you’re wondering what life looks like on the other side, what happens after trauma treatment covers what recovery and reintegration can realistically look like, because the goal isn’t just symptom reduction. It’s getting your life back.
How Residential Treatment Accelerates Healing
Trying to heal deep-seated trauma while managing the stress of daily life is incredibly difficult. Residential trauma treatment allows you to step out of your environment and focus 100% on recovery. Without daily triggers, your nervous system finally gets the chance to downregulate.
We use evidence-based modalities designed to rewire the brain and restore safety in the body, including:
- Eye Movement Desensitization and Reprocessing (EMDR): Reprocesses memories so they no longer trigger a fight-or-flight response.
- Somatic Experiencing: A body-focused approach to release physical tension stored from past events.
- Cognitive Behavioral Therapy (CBT): Helps reframe negative thought patterns and catastrophic thinking.
- Dialectical Behavior Therapy (DBT): Builds skills for emotional regulation and distress tolerance.
- Holistic Therapies: Yoga and mindfulness to safely reconnect you with your body.
Your Pain is Valid
Recognizing the signs you need trauma therapy (beyond PTSD) is a brave step. You do not need a tragic backstory or a total breakdown to justify seeking help.
If you are tired of merely coping and are ready to start living, we are here to support you. Your mental health matters. Contact Kinder in the Keys today for a confidential assessment, and let’s help you leave survival mode behind.
Ready to Heal from Trauma in a Safe, Supportive Space?
Discover trauma-informed care designed for women, with evidence-based therapies that help you process, heal, and reclaim your sense of safety and control.
